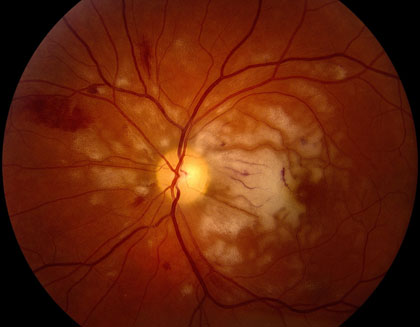
Ocular Trauma
/What is Ocular Trauma?
Generally, ocular trauma refers to an injury to the structures of the eye by a foreign object or chemical. Low energy blunt trauma (e.g., bump head getting out of the car) may cause minimal damage while high energy trauma (e.g., a projectile) may have more severe results. Prompt evaluation and treatment of damage to the back of the eye (the retina) may allow preservation and restoration of vision.
Diagnosis
Trauma may result in a number of conditions including retinal detachment, macular pucker, cataract, glaucoma and uveitis. With each of these conditions there is a risk of blindness. If you have experienced trauma, it is best to suspect an eye injury and report it to your eye doctor, immediately. Following an eye injury, the mildest pain and most minimal vision loss may require prompt treatment. If a sliver enters the eye, as a result of metal grinding or woodcutting, for example, the foreign body might result in loss of the eye, completely, if left untreated. Special diagnostic tests, used to localize damage to the eye, following trauma, include high-resolution digital fluorescein angiography, ultrasonography, and electroretinography.
Who is at risk?
Over 2.5 million Americans suffer eye trauma, annually, with over 10% experiencing permanent vision loss. While vision loss is often acute, degeneration may occur months or years later. Everyone, at any age, is at risk for ocular trauma. A simple bump to the head may cause traumatic optic neuropathy, which may result in blindness if not treated with steroids or surgery. Children and young adults who play sports, fight, or use BB-guns etc. are at an increased risk.
Signs and Symptoms
Do not assume that minimal trauma equals minimal damage. Even a mild bump to the head, resulting in minimal redness and zero vision loss, may lead to blindness. Classic symptoms, associated with trauma, include swelling around the eye, dropping of the eyelid, bleeding/bruising, or pupil dilation. However, some of the most severe cases may not show any symptoms. Therefore, if you note any vision change or have a history of trauma, with or without symptoms, a careful examination by your eye doctor is necessary.
Treatment
Obvious complications, as a result of blunt trauma, include eye inflammation (traumatic iritis), damage to the pupil (traumatic mydriasis), and blood in the front of the eye (hyphema). A careful microscopic exam, by your eye doctor, will reveal these conditions. Management normally includes the use of anti-inflammatory drops (NSAIDS and steroids) and dilation drops (cycloplegics) for up to two weeks. Other signs of trauma include a deepening of the anterior chamber (angle recession, iridodialysis, lens subluxation), low eye pressure (possible eye rupture or retinal detachment), poor light response at the pupil (aka, APD associated with damage to the retina, macular or optic nerve) and the presence of pigment cells in the anterior vitreous (retinal dialysis or tear). If macular changes occur, referral is necessary. Urgent treatments include pneumatic displacement of subretinal blood, surgical repair of a traumatic macular hole or retinal detachment and the corresponding treatment of abnormal blood vessels (choroidal neovascularization, CNV) with anti-VEGF therapy (eg, Avastin).